Crypto Trading Success Mastering Technical Analysis
Understanding Technical Analysis Tools to Maximize Your Crypto Trading Success is crucial for navigating the volatile cryptocurrency market. This guide dives deep into the world of charts, indicators, and patterns, empowering you to make informed decisions and potentially boost your trading profits. We’ll explore essential tools, from basic charts to advanced techniques, and provide practical strategies for incorporating them into your trading approach.
Technical analysis is a cornerstone of successful crypto trading. It’s not about predicting the future, but rather identifying potential trends and patterns in historical data. By understanding how price movements and volume relate, traders can identify opportunities and mitigate risks, ultimately maximizing their chances of success in the dynamic crypto market. This comprehensive guide equips you with the knowledge and tools to excel in your crypto journey.
Introduction to Technical Analysis in Crypto Trading

Source: medium.com
Technical analysis in cryptocurrency trading is the process of using historical price and volume data to identify patterns and predict future price movements. It’s a crucial tool for traders aiming to make informed decisions and potentially maximize their profits. This approach doesn’t rely on fundamental factors like company performance or economic indicators; instead, it focuses on the market’s collective sentiment as reflected in price charts and indicators.
Mastering technical analysis is key to successful crypto trading, but did you know that understanding the power of natural remedies like clove and black nutmeg might also play a role in your overall well-being? Check out Unlock the Secret Health Powers of Clove and Black Nutmeg for insights into these incredible spices. Ultimately, a balanced approach to both your trading strategies and overall health is crucial for long-term success in the crypto market.
By understanding and interpreting these patterns, traders can anticipate potential trends and adjust their strategies accordingly.Technical analysis isn’t a foolproof method for predicting the future. It relies on identifying recurring patterns and making educated guesses based on past data. However, it can provide valuable insights and help traders manage risk more effectively. While no system guarantees success, skilled traders leverage technical analysis to increase their odds of positive outcomes in the volatile crypto market.
Core Principles of Technical Analysis
Technical analysis rests on several core principles. These include the belief that market trends have a tendency to repeat themselves, and that price movements are driven by collective investor sentiment, which can be reflected in chart patterns and indicators. The analysis relies heavily on the concept of supply and demand dynamics, with price action interpreted as the interplay of these forces.
Understanding the psychology behind market behavior is also a significant aspect of successful technical analysis, allowing traders to anticipate reactions to significant price changes.
Methodologies Used in Technical Analysis, Understanding Technical Analysis Tools to Maximize Your Crypto Trading Success
Various methodologies underpin technical analysis. These include chart patterns recognition, trend identification, and the use of technical indicators. Chart patterns are recurring formations that can suggest potential price movements. Trend identification involves determining the prevailing direction of the market (uptrend, downtrend, or sideways movement). Technical indicators are mathematical calculations derived from price and volume data that provide insights into market sentiment and potential price changes.
A crucial element is recognizing support and resistance levels, which represent areas where prices have historically tended to reverse direction.
Importance of Technical Analysis for Crypto Trading Success
Technical analysis is vital for crypto trading success due to the inherent volatility and unpredictable nature of the cryptocurrency market. It enables traders to identify potential entry and exit points, assess market sentiment, and manage risk more effectively. The ability to spot trends and patterns empowers traders to adapt to market fluctuations and make informed decisions based on historical data.
This allows for a more disciplined approach, which is critical for mitigating the risks associated with high volatility. By leveraging technical analysis tools, traders can increase their chances of positive outcomes.
Different Types of Technical Analysis Tools
Understanding various tools is crucial for effective technical analysis. Different tools offer varying perspectives on the market and can help in understanding different aspects of market sentiment.
| Tool Type | Description | Example |
|---|---|---|
| Charts | Visual representations of price and volume data over time. | Candlestick charts, line charts, bar charts. |
| Indicators | Mathematical calculations derived from price and volume data that provide insights into market sentiment and potential price changes. | Moving averages, Relative Strength Index (RSI), Bollinger Bands. |
| Pattern Recognition | Identifying recurring formations in price charts that can suggest potential price movements. | Head and shoulders, double tops/bottoms, triangles. |
Essential Crypto Trading Charts
Navigating the dynamic world of crypto trading hinges on effectively interpreting price movements. Understanding the various chart types available, and how to glean valuable insights from them, is paramount for success. This section delves into essential chart types, their interpretation, and how to identify crucial market signals.Cryptocurrency charts, much like stock market charts, visualize price action over time.
They reveal trends, support and resistance levels, and potential trading opportunities. By mastering these visual tools, traders can make more informed decisions and enhance their chances of profitable trades.
Chart Types in Crypto Trading
Different chart types offer unique perspectives on price action. Each type emphasizes specific aspects of price movements, enabling traders to spot various patterns and signals.
- Line Charts: These charts display the closing price of an asset over time, connected by a line. They provide a simplified overview of the overall trend, allowing traders to quickly assess the general direction of the market. Identifying the general uptrend or downtrend becomes straightforward, and they’re especially helpful for spotting long-term trends.
- Bar Charts: Bar charts show the open, high, low, and closing prices of an asset for a specific period. Each bar represents a time frame, providing a detailed picture of price volatility. They reveal the range of price movements within a given period and help in identifying the strength of buying or selling pressure.
- Candlestick Charts: Candlestick charts, a popular choice, visually represent the open, high, low, and closing prices of an asset. The “body” of the candlestick indicates the opening and closing prices, while the “wick” or “shadow” signifies the high and low. They offer more detailed information than line charts and provide a clearer picture of price action, highlighting potential reversal patterns and momentum.
Interpreting Price Action on Different Charts
Understanding how to interpret price action is crucial for extracting actionable insights from any chart type. This involves recognizing patterns and using them to predict future price movements.
- Trends: Upward trends, downward trends, and sideways trends can be identified on all chart types. On line charts, a steadily rising line suggests an uptrend, while a consistently declining line indicates a downtrend. Bar charts highlight the price range within a given time period, making it easier to spot the overall trend. Candlestick charts depict the strength of price movements, revealing bullish or bearish momentum, and thus confirming trends.
- Support and Resistance Levels: Support levels are price points where the price has historically bounced back from. Resistance levels, conversely, represent price points where the price has previously encountered significant selling pressure. Identifying these levels on all chart types helps traders anticipate potential price reversals and adjust their trading strategies accordingly. For instance, if the price breaks through a support level, it could indicate a further downward trend.
Examples of Trend Identification
Identifying trends on various charts can help predict potential price movements.
- Line Chart Example: A steadily upward sloping line on a daily timeframe line chart of Bitcoin suggests an overall bullish trend.
- Bar Chart Example: A series of bar charts with higher highs and higher lows over several days on a trading platform signifies a potential upward trend.
- Candlestick Chart Example: A sequence of green candlestick bodies with increasing highs and lows on a 4-hour timeframe of Ethereum shows a possible uptrend.
Common Chart Patterns
Recognizing chart patterns can help predict future price movements.
| Pattern | Description | Implications |
|---|---|---|
| Head and Shoulders | A reversal pattern consisting of three peaks, with the middle peak (head) higher than the other two (shoulders). | Potential bearish reversal. |
| Triangles | A consolidation pattern characterized by converging trend lines. | Potential continuation of the prevailing trend or a breakout in the opposite direction. |
Key Technical Indicators
Technical indicators are tools that analyze historical price and volume data to identify patterns and potential future price movements in cryptocurrencies. They provide a quantitative perspective beyond just visual chart patterns, assisting traders in making more informed decisions. Understanding how these indicators function and their limitations is crucial for effective crypto trading.
Moving Averages
Moving averages smooth out price fluctuations, revealing the overall trend direction. They help identify support and resistance levels. Different periods for calculating the average (e.g., 20-day, 50-day, 200-day) provide varying levels of smoothing and responsiveness to price changes.
Mastering technical analysis tools is key to successful crypto trading, but managing stress is equally important. Sometimes, finding the right focus can feel like a monumental task. Have you considered natural remedies like ginger for stress relief and improved focus? Check out this fascinating article on Can Ginger Really Help You Manage Stress and Improve Focus?
to see if it could help you. Ultimately, a calm mind and sharp analysis are crucial to navigating the volatile crypto market.
A simple moving average (SMA) is calculated by averaging the closing prices over a specific period.
The 50-day moving average is often used as a short-term trend indicator, while the 200-day moving average acts as a longer-term trend indicator. A bullish trend is suggested when the price is above its moving averages, and vice versa for a bearish trend. However, moving averages are lagging indicators, meaning they react to price changes after they’ve occurred.
They don’t predict future movements but rather confirm existing trends.
Relative Strength Index (RSI)
The RSI measures the magnitude of recent price changes to evaluate overbought or oversold conditions. A reading above 70 often suggests an asset is overbought, potentially leading to a price correction. Conversely, a reading below 30 suggests an asset is oversold, potentially signaling a buying opportunity.
RSI = 100 – (100 / (1 + RS)) where RS = Average of “up” price change / Average of “down” price change.
RSI values are typically calculated over 14 periods. The RSI is helpful for identifying potential reversals, but it can be prone to whipsaws (sudden, sharp price movements) in highly volatile markets.
Moving Average Convergence Divergence (MACD)
The MACD uses two moving averages to identify momentum and potential turning points. It plots the difference between two moving averages, usually a 12-day and 26-day exponential moving average (EMA). A histogram, which visually represents the difference, can highlight potential buy or sell signals.
MACD = 12-day EMA – 26-day EMA
The MACD’s strength lies in its ability to highlight momentum shifts. However, it can generate false signals, particularly in trending markets. The MACD often needs to be used in conjunction with other indicators and chart patterns for confirmation.
Table of Technical Indicators
| Indicator | Calculation | Interpretation | Strengths | Limitations |
|---|---|---|---|---|
| Moving Average (e.g., 20-day SMA) | Average of closing prices over a specified period | Trend identification, support/resistance | Simple, clear trend signals | Lagging indicator, may not capture short-term fluctuations |
| RSI (Relative Strength Index) | Magnitude of recent price changes | Overbought/oversold conditions | Identifies potential reversals | Prone to whipsaws, needs confirmation |
| MACD (Moving Average Convergence Divergence) | Difference between two EMAs (e.g., 12-day and 26-day) | Momentum and turning points | Highlights momentum shifts | Can generate false signals, needs confirmation |
Tools for Analyzing Trading Volume and Volatility: Understanding Technical Analysis Tools To Maximize Your Crypto Trading Success
Understanding trading volume and volatility is crucial for successful crypto trading. These factors provide insights into market sentiment and the potential for price fluctuations. Analyzing volume and volatility helps traders identify potential trends, assess market strength, and manage risk effectively. By understanding how volume and volatility interact, you can make more informed trading decisions and improve your overall profitability.
Impact of Volume on Price Movements
Volume data reflects the overall trading activity in a cryptocurrency. High trading volume often accompanies significant price movements, indicating strong market participation and increased interest in the asset. Conversely, low volume can signal a lack of conviction and potentially weaker price action. This correlation between volume and price action is fundamental to technical analysis. For example, a strong upward price movement accompanied by high volume suggests that buyers are actively pushing the price higher, increasing the likelihood of continued upward momentum.
Identifying Significant Volume Spikes and Patterns
Identifying significant volume spikes and patterns is key to understanding market sentiment and potential price reversals. Tools like volume profiles, which visualize the trading volume over time, can help traders identify periods of high or low volume. Volume bars, which display the volume traded during each time interval, can also highlight significant spikes. Analyzing volume patterns in conjunction with price charts helps traders understand the underlying market dynamics and make more informed trading decisions.
For instance, a sudden surge in volume at a specific price level could indicate a breakout or reversal.
Influence of Volatility on Trading Decisions
Volatility measures the degree of price fluctuation over a given period. High volatility indicates significant price swings, increasing the risk of substantial losses but also the potential for substantial profits. Low volatility suggests a stable market, reducing risk but potentially limiting profit opportunities. Understanding the volatility levels is crucial for risk management. Traders must adjust their strategies based on the prevailing volatility levels.
Strategies for Managing Risk Related to Volatility
Managing risk related to volatility is paramount in crypto trading. Stop-loss orders help limit potential losses by automatically selling an asset when it reaches a predetermined price level. Diversification across different cryptocurrencies can also mitigate risk, spreading capital across multiple assets with varying volatility profiles. Hedging strategies, which involve using other financial instruments to offset potential losses, can also be employed.
For example, if a trader anticipates high volatility, they might choose to use stop-loss orders or reduce their position size to limit potential losses.
Table Contrasting Different Volume and Volatility Indicators
| Indicator | Description | How it Works | Strengths | Weaknesses |
|---|---|---|---|---|
| Volume Profile | Visual representation of trading volume over time. | Shows distribution of volume across different price levels. | Identifies areas of strong buying or selling pressure. | Requires careful interpretation and may not be effective in highly volatile markets. |
| Volume Bars | Displays volume traded during each time interval. | Shows the trading activity for a given period. | Helps identify significant volume spikes and patterns. | Can be cluttered and may require combining with other indicators for comprehensive analysis. |
| Average True Range (ATR) | Measures price volatility over a specified period. | Calculates the average range of price fluctuations. | Provides a quantitative measure of volatility. | Doesn’t account for specific market conditions or sentiment. |
| Bollinger Bands | Plots bands above and below a moving average. | Indicates volatility levels by showing the range of expected price movements. | Identifies potential areas of overbought or oversold conditions. | Requires careful consideration of the moving average period used. |
Identifying Support and Resistance Levels

Source: ytimg.com
Support and resistance levels are crucial concepts in technical analysis, acting as vital signposts for potential price movements in the crypto market. Understanding how to identify and interpret these levels allows traders to anticipate potential reversals, set profitable entry and exit points, and manage risk effectively. They represent price zones where buying or selling pressure is often concentrated, creating areas of potential support or resistance.Identifying these levels on charts is key to making informed trading decisions.
Knowing where these levels are located provides valuable insight into market sentiment and potential future price action. By understanding the dynamics of support and resistance, traders can develop more sophisticated trading strategies and capitalize on opportunities.
Methods for Determining Support and Resistance
Support and resistance levels can be determined through various methods, each with its own strengths and limitations. Different approaches often yield similar results but with varying degrees of precision. The selection of the appropriate method depends on the specific trading strategy and market conditions.
- Trend Lines: Trend lines are drawn on charts to connect a series of highs or lows, indicating the prevailing trend. A support level is established where the price has previously bounced off a downtrend, while a resistance level is formed where the price has repeatedly failed to break through an uptrend. These lines offer a visual representation of the market’s direction and can be used to predict potential support or resistance points.
For instance, if a price consistently bounces off a specific trend line on a downtrend, it indicates a potential support level.
- Fibonacci Levels: Fibonacci retracements and extensions are based on mathematical ratios derived from the Fibonacci sequence. These ratios can be used to identify potential support and resistance levels. Significant price levels that correspond to Fibonacci ratios frequently show up as areas where price action reverses. For example, a 50% Fibonacci retracement level may serve as a support level after a substantial price drop.
- Moving Averages: Moving averages are calculated by averaging the price of an asset over a specific period. These averages can act as support or resistance levels, especially when they coincide with other indicators or chart patterns. For instance, a 200-day moving average is often seen as a strong support or resistance level, depending on the overall trend.
- Volume Analysis: Observing trading volume alongside price action can enhance the reliability of support and resistance identification. High volume in the vicinity of a support or resistance level often suggests significant interest at that price point. This increased volume could signify a stronger potential for price action to reverse.
Comparing Support and Resistance Determination Methods
| Method | Description | Strengths | Weaknesses |
|---|---|---|---|
| Trend Lines | Connecting highs or lows to indicate trend | Simple to identify, visually clear | Can be subjective, less precise than other methods |
| Fibonacci Levels | Based on mathematical ratios | Provides potential support/resistance levels, often accurate | Can be overused, can give false signals |
| Moving Averages | Averaging price over a period | Provides a smoother view of the trend | Can lag behind price action, may not always coincide with support/resistance |
| Volume Analysis | Observing trading volume around price levels | Can confirm strength of support/resistance | Volume alone isn’t sufficient for accurate identification |
Chart Patterns and Their Implications
Chart patterns are recurring visual formations on price charts that can potentially signal future price movements. Understanding these patterns is crucial for crypto traders, allowing them to identify potential entry and exit points, manage risk, and make more informed decisions. Recognizing these formations, however, requires careful observation and a solid understanding of the underlying market dynamics.
Common Chart Patterns
Chart patterns often reveal underlying market sentiment and momentum. These patterns, like fingerprints, can offer insights into the potential direction and magnitude of price changes.
- Head and Shoulders: This pattern is characterized by a peak (the head) flanked by two lower peaks (the shoulders). A breakdown below the neckline, the line connecting the lows of the shoulders, often signals a potential downward trend. The inverse (a head and shoulders pattern with a neckline break above) signals a potential upward trend.
- Double Tops/Bottoms: These patterns are characterized by two consecutive peaks (tops) or troughs (bottoms) with similar highs or lows. A break below the support level (for double bottoms) or above the resistance level (for double tops) often suggests a reversal in trend. The key is recognizing the similarity in the peaks/troughs.
- Triangles: Triangles are characterized by converging trend lines, either upward or downward. A breakout above or below the trend lines often signifies the direction of the next price movement. The strength of the breakout and the volume associated with it can further strengthen the prediction.
Interpreting Chart Patterns for Informed Trading Decisions
Interpreting chart patterns requires a nuanced approach. It’s crucial to consider the volume and price action accompanying the pattern. For example, a strong breakout with high trading volume often suggests a more significant price movement.
Example Interpretations
Imagine a head and shoulders pattern forming on the Bitcoin chart. The neckline is broken, and the price starts to fall below it. This could suggest a potential downtrend. However, the trader should carefully consider the overall market sentiment and any other technical indicators before making a trade decision. Similarly, a double bottom pattern might indicate a potential rebound.
Table of Chart Patterns and Possible Outcomes
| Chart Pattern | Description | Potential Outcome |
|---|---|---|
| Head and Shoulders | A peak (head) flanked by two lower peaks (shoulders). | Breakdown below the neckline suggests a potential downtrend. |
| Double Tops | Two consecutive peaks with similar highs. | Break below the resistance level suggests a potential downtrend. |
| Double Bottoms | Two consecutive troughs with similar lows. | Break above the support level suggests a potential uptrend. |
| Triangles | Converging trend lines. | Breakout above or below the trend lines suggests the direction of the next price movement. |
Risk Management Strategies for Crypto Trading
Cryptocurrency trading, while offering potentially high rewards, carries significant risks. Understanding and implementing effective risk management strategies is crucial for long-term success. A well-defined approach to managing risk can help mitigate losses and protect capital, allowing traders to navigate the volatility of the market with greater confidence.A proactive risk management plan goes beyond just looking at technical indicators.
It involves setting clear limits, understanding your own trading psychology, and consistently adapting your strategies based on market conditions. By combining technical analysis with robust risk management, traders can significantly improve their chances of profitability in the crypto market.
Position Sizing
Proper position sizing is fundamental to risk management. It dictates the percentage of your trading capital allocated to each trade. Over-leveraging in a single trade can quickly wipe out your account if the trade goes against you.
- A common approach is to limit each trade to a pre-determined percentage of your trading capital, typically 1-2%. This approach helps to prevent significant losses from a single trade. For example, if your trading capital is $10,000, a 1% position size would limit each trade to $100.
- Adjusting position size based on the perceived risk of a trade is also essential. A highly volatile cryptocurrency or a trade with a limited historical data set should be assigned a smaller position size to mitigate potential losses. This is often referred to as “risk-adjusted position sizing”.
Stop-Loss Orders
Stop-loss orders are crucial for limiting potential losses. They automatically close a trade when the price reaches a predetermined level.
- Setting appropriate stop-loss levels is critical. These levels should be placed below potential support levels or above potential resistance levels, based on your technical analysis of the asset’s price chart. Avoid placing stop-loss orders too close to the current market price as this can trigger a trade when the price moves only slightly.
- A common mistake is setting stop-loss orders too close to the entry point. This can result in significant losses if the market moves against you unexpectedly. For example, if you buy Bitcoin at $29,000 and set a stop-loss at $28,000, a sharp price drop could lead to substantial losses.
Diversification
Diversifying your crypto holdings across various cryptocurrencies and asset classes is a key risk management technique. It reduces the impact of a single cryptocurrency’s poor performance on your overall portfolio.
- Diversification is about reducing your exposure to any one particular asset. If a significant portion of your portfolio is invested in a single cryptocurrency, you could experience substantial losses if that cryptocurrency experiences a significant downturn. For instance, an investor with 80% of their portfolio invested in Bitcoin is significantly more vulnerable to market fluctuations than an investor who has diversified their portfolio.
- By spreading your investments across various cryptocurrencies, you can reduce your overall risk. This includes different types of cryptocurrencies, such as stablecoins, altcoins, and NFTs. A diversified portfolio should include different tokens and project types.
Implementing Strategies with Technical Analysis
Technical analysis tools can help in implementing these strategies. For example, identifying potential support and resistance levels using candlestick charts can inform your position sizing decisions.
- When a cryptocurrency breaks a major support level, it might indicate a potential downtrend. This could influence your position sizing to reduce risk.
- Conversely, if a cryptocurrency reaches a significant resistance level, it might suggest a period of consolidation or a potential reversal. This could influence your position sizing to increase your risk tolerance or reduce exposure.
Advanced Technical Analysis Techniques
Beyond the fundamental and intermediate techniques, advanced technical analysis methods offer a deeper dive into market dynamics. These approaches, while often more complex, can provide valuable insights for identifying potential trading opportunities. They incorporate various factors, including market psychology and historical patterns, to predict future price movements. However, it’s crucial to remember that no technical analysis method guarantees success, and advanced techniques should be used in conjunction with risk management strategies.Advanced techniques often involve complex calculations and interpretations of market data, demanding a deeper understanding of the underlying principles.
While basic techniques might focus on price action and simple indicators, advanced methods delve into more nuanced aspects of market behavior. Careful consideration and testing of these techniques in a simulated or demo trading environment are essential before applying them to real capital.
Elliott Wave Theory
Elliott Wave Theory postulates that market movements unfold in predictable wave patterns, mirroring human psychology and emotional responses to market events. These waves are grouped into five upward waves and three downward waves, reflecting alternating periods of optimism and pessimism. Understanding these wave patterns can help traders anticipate potential price reversals and support/resistance levels.An example of an application is recognizing a corrective wave, followed by an impulsive wave, to identify potential buying opportunities.
This approach is more predictive than simple trend identification. It requires a considerable amount of practice to discern the waves accurately, and traders should avoid over-reliance on this theory as a sole predictor.
Fibonacci Analysis
Fibonacci analysis utilizes a series of numbers (the Fibonacci sequence) to identify potential support and resistance levels. These levels are calculated based on mathematical relationships within the sequence, believed to reflect inherent patterns in market behavior. Fibonacci retracements, extensions, and arcs can indicate areas where prices might pause or reverse direction.A practical example of Fibonacci analysis is using Fibonacci retracement levels to pinpoint potential support zones during a downtrend.
If the price retraces to a significant Fibonacci level, it might indicate a pause in the downward movement or a potential buying opportunity. This approach, while helpful in identifying potential turning points, should not be treated as a sole determinant of trading decisions.
Comparison with Basic Methods
While basic methods like trend lines and moving averages offer a straightforward way to understand price action, advanced techniques provide a more comprehensive and nuanced perspective. Elliott Wave Theory and Fibonacci analysis consider market psychology and underlying patterns, which basic methods often overlook. However, advanced methods require a deeper understanding of the underlying principles and can be more subjective in interpretation.
| Method | Focus | Complexity | Reliability |
|---|---|---|---|
| Trend Lines/Moving Averages | Price action, short-term trends | Low | Moderate |
| Elliott Wave Theory | Market psychology, long-term patterns | High | Variable |
| Fibonacci Analysis | Mathematical relationships, support/resistance | Medium | Moderate |
Practical Application of Tools for Success
Turning technical analysis from theory into profitable trading requires a practical approach. This involves understanding how to integrate the tools and indicators discussed into a structured trading plan. A crucial aspect of this is understanding that technical analysis is not a crystal ball, but a powerful tool to identify potential trading opportunities and increase your chances of success in the volatile crypto market.Effective application of technical analysis demands a step-by-step approach, blending the insights gleaned from charts and indicators with a well-defined risk management strategy.
By carefully considering support and resistance levels, chart patterns, and volume trends, traders can make more informed decisions, ultimately maximizing their potential returns while minimizing risks.
Steps in Using Technical Analysis Tools
Applying technical analysis effectively involves a series of steps. These steps should be consistently followed to ensure a disciplined and profitable approach to trading. A methodical process allows for more accurate interpretation of market signals and lessens the likelihood of impulsive decisions.
Mastering technical analysis tools is key to successful crypto trading, but did you know that a good night’s sleep can significantly boost your focus and decision-making? This is crucial for interpreting charts and market trends effectively. For example, incorporating natural sleep aids like cinnamon and cardamom, as detailed in The Amazing Role of Cinnamon and Cardamom in Promoting Better Sleep Quality , can improve your overall trading performance.
Ultimately, a combination of sharp analytical skills and good sleep hygiene is the winning formula for crypto success.
- Identify the time frame: Choosing the appropriate time frame for analysis is crucial. Short-term charts capture intraday fluctuations, while longer-term charts provide a broader view of market trends. Different trading strategies will require different timeframes for analysis, ranging from intraday to weekly or monthly.
- Select relevant indicators: Select the technical indicators most relevant to the specific trading strategy. For example, if focusing on short-term momentum, indicators like RSI or MACD might be more pertinent than long-term trend indicators like moving averages.
- Analyze chart patterns: Recognize chart patterns that suggest potential price movements. Understanding patterns like head and shoulders, triangles, or flags helps predict future price behavior. Recognizing patterns in candlestick charts, for example, can identify potential buying or selling opportunities.
- Establish support and resistance levels: Identify key support and resistance levels on the chart. These levels act as significant price points where the price may reverse or consolidate. Knowing these points can help to place buy or sell orders strategically.
- Evaluate trading volume: Consider the trading volume accompanying price movements. High volume during price movements often signals strong conviction, suggesting a higher likelihood of the trend continuing. Low volume often signals uncertainty, potentially leading to a pause in the trend.
- Integrate indicators and patterns: Combine the insights from different indicators and patterns to form a more comprehensive picture of the market. A confirmation from multiple indicators increases the reliability of the trading signal.
- Develop a trading plan: Develop a detailed trading plan incorporating the analysis. The plan should specify entry and exit points, stop-loss orders, and profit targets based on the identified opportunities. A solid trading plan is essential for disciplined execution and risk management.
Integrating Technical Analysis into a Trading Strategy
Integrating technical analysis into a trading strategy involves more than just applying indicators. A comprehensive approach considers risk management, market conditions, and personal trading style.
- Establish entry and exit points: Use technical analysis to determine optimal entry and exit points. Entry points should be supported by multiple indicators, and exit points should consider profit targets or stop-loss levels.
- Set stop-loss orders: Define stop-loss orders based on technical analysis to limit potential losses. Stop-loss orders are essential to manage risk and prevent significant capital loss.
- Consider market sentiment: Supplement technical analysis with an understanding of market sentiment. News events, social media trends, and overall market conditions can impact price movements.
- Develop a risk management strategy: A robust risk management strategy is crucial. This involves setting position sizes and defining risk tolerance levels. It also entails adjusting trading positions based on the identified risk.
Successful Trading Strategies
Successful trading strategies often combine fundamental analysis with technical analysis. Examples include:
- Breakout strategies: These strategies capitalize on price breaks above or below significant resistance or support levels.
- Trend-following strategies: These strategies focus on identifying and riding prevailing trends, using indicators to confirm and manage positions.
- Swing trading strategies: These strategies aim to capitalize on short-term price swings by analyzing chart patterns and indicators.
Applying Technical Analysis Tools: A Step-by-Step Guide
| Technical Analysis Tool | Step 1: Identification | Step 2: Analysis | Step 3: Interpretation |
|---|---|---|---|
| Moving Averages | Identify relevant timeframes and moving averages (e.g., 20-day, 50-day). | Observe the movement of the moving average relative to the price. | Interpret the crossing or convergence of moving averages as potential signals. |
| Relative Strength Index (RSI) | Calculate the RSI for a chosen timeframe. | Analyze RSI values for overbought or oversold conditions. | Confirm potential reversal points with other indicators. |
| Support and Resistance Levels | Identify key support and resistance levels on the chart. | Examine price action at these levels. | Interpret price reactions at support and resistance as potential trading signals. |
Last Point
In conclusion, mastering technical analysis is a vital step in maximizing your crypto trading success. This guide provided a roadmap for understanding various tools and strategies, from interpreting charts and indicators to managing risk. By integrating these insights into your trading strategy, you’ll be better equipped to navigate the complexities of the crypto market. Remember, consistent learning and adaptation are key to long-term success in this ever-evolving landscape.
FAQ Guide
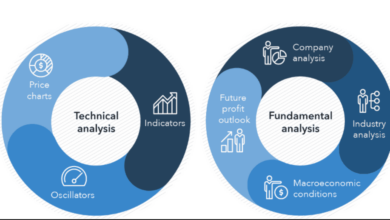
What is the difference between technical and fundamental analysis?
Technical analysis focuses on historical price and volume data, while fundamental analysis considers underlying factors like company performance, market trends, and news events.
How can I determine if a technical indicator is reliable?
A reliable indicator is consistent over time, and it’s best used in conjunction with other tools and indicators, not in isolation. Look for indicators with clear definitions, calculations, and established applications.
How can I use technical analysis to manage risk?
Technical analysis helps identify potential support and resistance levels, which can aid in setting stop-loss orders and managing positions to limit potential losses.
What are some common pitfalls to avoid when using technical analysis?
Over-reliance on a single indicator, ignoring fundamental factors, and not adapting to market changes are common pitfalls to avoid. Always combine technical analysis with other market research and your own trading strategy.